A Physician with a Passion

Thanks to the advocacy of Terri Finkel, MD, PhD, Le Bonheur interim pediatrician-in-chief, legislation was passed in Tennessee expanding access to whole genome sequencing in critically ill children with TennCare coverage.
Years ago, Terri Finkel, MD, PhD, lobbied before a local government board to block development of a Denver wetlands area, after she researched and found a particular species of wildlife there needed protecting. While she describes herself as “not particularly political,” she also admits, “when I get passionate about something, I research it to death.”
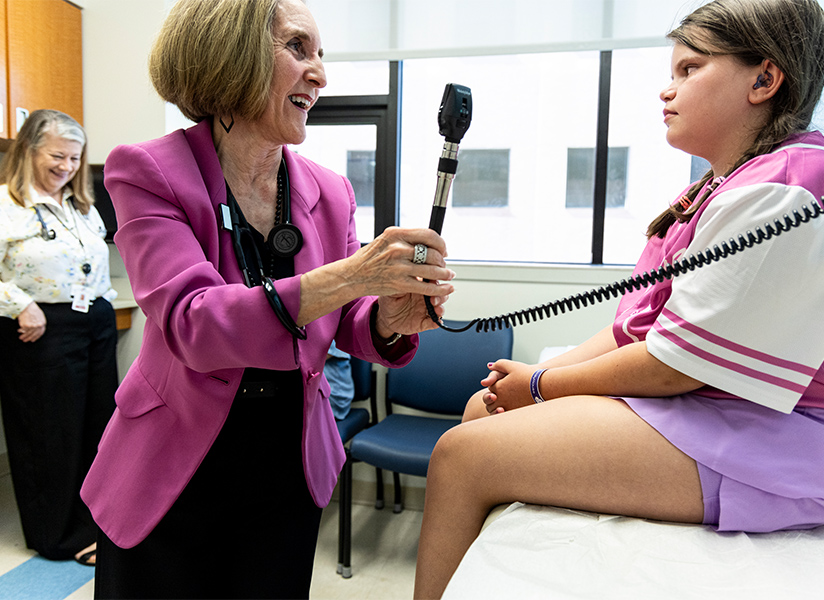
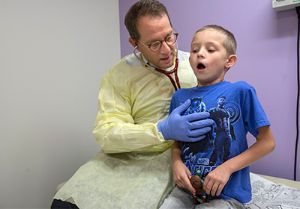
Above left, Terri Finkel, MD, PhD, examines a patient in clinic. A rheumatologist by training, Finkel states this expanded access to whole genome sequencing could reduce time to diagnosis and lower the burden of suffering for children and families.
The wetlands eventually were developed, but the species was protected. That was her only brush with a government body, until 2024 when she stood before the Tennessee legislature armed with her customary copious research and a passion to help seriously ill children.
Finkel advocated before the state House and Senate for legislation to require TennCare coverage for rapid whole genome sequencing of newborns when certain criteria are met. This, she explained to the lawmakers, would give physicians the power to diagnose babies sooner and eliminate the pain and suffering of months and possibly years of testing to get a diagnosis.
The legislation passed unanimously and was signed into law May 28, making Tennessee one of 11 states to have this health care benefit. In nine of those states, rapid whole genome sequencing is an approved benefit only for infants. Tennessee joined Minnesota in extending the benefit from birth to age 21.
“This is a life-changing event in Tennessee,” Finkel says. “It is a benefit that the citizens of Tennessee now have that will save the lives of many children over the years. And it affirms the importance of access to genetic sequencing as part of our diagnostic armamentarium.”
Finkel is the interim pediatrician-in-chief at Le Bonheur Children’s Hospital and a professor and the interim chair of the Department of Pediatrics at the University of Tennessee Health Science Center (UTHSC). A pediatric rheumatologist, she is passionate about diagnosing, treating and easing the suffering of infants and children with rheumatological diseases.
Whole genome sequencing organizes the entire DNA sample that makes up an individual human genome into a file of letters that then can be examined for mutations that characterize certain diseases. Rapid testing generates results within 15 days from the date of receipt of the sample, with preliminary results as early as seven days.
“The rapid whole genome sequence allows us to know whether there are variants in known genes, whether there are specific proteins that are working in a child who has a critical illness,” Finkel explains. Early and rapid testing can translate to earlier and faster diagnosis and treatment.
Specific criteria make a child eligible for the testing, such as presenting with an acute or complex illness of unknown cause, abnormal laboratory tests or chemistry profiles suggesting a genetic disease or congenital anomalies involving at least two organ systems. However, physicians can also apply evidence-based medical necessity criteria.
“The law just has to do with if the child is not responding to treatment as we anticipate, which makes it very user friendly in the sense that we can use our judgment as physicians as to which children are most likely to benefit from this test,” Finkel says.
Her extensive history working with critically-ill children and their families propelled her to advocate for better interventions for children who might otherwise languish in the process of diagnosis.
After becoming aware of the effort in Michigan to pass similar legislation, “I began researching how I could make that happen in Tennessee,” she says. Similar efforts by others in Tennessee had stalled, primarily because of the cost associated with rapid whole genome sequencing.
Earlier this year, Finkel connected with David Mills, director of Government Relations for UTHSC and together they investigated the opportunity to renew the effort.
State Representative Brock Martin and state Senator Richard Briggs were the sponsors of the legislation, House Bill 1826 and Senate Bill 1762.
“They asked me to write a justification based on what we knew from three other big studies, one in California, the one in Michigan and one in in Florida, which had all passed this bill,” Finkel says. “Based on those studies, it showed that not only was it cost effective, but it saved and generated money.”
“In other words, the cost of the test is offset by the fact that you have children in the hospital fewer days, and they need fewer expensive, painful, prolonged testing,” she explains. “And so, aside from the actual cost saving, there's the saving of worry and lost work time and suffering of both families and the children.”
Finkel wrote letters with the message the legislation would save lives without excessive costs to the state. She addressed both the house and the senate in her capacity as a physician who cares for infants and children who could benefit from the testing.
In addition to invaluable support from Mills, Maureen O’Connor, vice president of Institutional Advancement at Le Bonheur Children’s Hospital, and Cary Whitworth, vice president of Government Relations and Advocacy for the UT System, as well as the Children's Hospital Association of Tennessee, St. Jude Children’s Research Hospital and Vanderbilt got behind the legislation. “This would not have been possible without the support of leadership at the university, the hospitals and the other health care entities,” she says.
The law went into effect July 1, 2024. Estimates are at least 55 children a year could be candidates for the test.
“This is going to take a while to get adopted,” Finkel says. “TennCare has to make policy, and we're going to work with them on that. And that can take a little while, and it's going to take a while for the hospitals to adopt it.”
Still, Finkel says, “It was one of the most remarkable things I've been involved in.”
Help us provide the best care for kids.
Le Bonheur Children's Hospital depends on the generosity of friends like you to help us serve 250,000 children each year, regardless of their family’s ability to pay. Every gift helps us improve the lives of children.
Donate Now