A Better Map
Transcranial magnetic stimulation (TMS) is safe, reliable and effective to map motor, speech and language function in young children with refractory epilepsy or a brain tumor, according to research published in Frontiers in Neurology by Le Bonheur Neuroscientist and Director of the TMS Laboratory Shalini Narayana, MS, MBBS, PhD. In 47 TMS motor mapping sessions, motor cortices were successfully mapped in 90% of children younger than 3 years old, and in 13 TMS language mapping sessions, language areas were located in 92% of children ages 5 to 6 years old. This is the largest known study reporting TMS mapping of motor cortices in toddlers and language cortices in preschool children. TMS maps can be used for presurgical planning to preserve language and motor function and provide a baseline for post-surgical changes in these functions.
“Accurate presurgical mapping of motor, speech and language cortices, while crucial for neurosurgical planning and minimizing post-operative functional deficits, is challenging in young children with neurological disease,” said Narayana. “Our data show that TMS can be a useful tool in mapping eloquent cortices in children with epilepsy or a brain tumor.”
TMS provides several advantages for mapping the language and motor areas of the brain in young children. Mapping is still possible with TMS even when patients are unable to fully cooperate due to disease or developmental delay. TMS is non-invasive, never requires sedation, does not require the patient to remain still and can be guided by previous MRI scans. For all of these reasons, TMS is a promising method for brain mapping for a young child for whom other methods, such as magnetoencephalography (MEG) and functional MRI (fMRI), have been unsuccessful. Without a viable functional mapping method, surgical options that could greatly improve cognitive function and quality of life may be delayed.
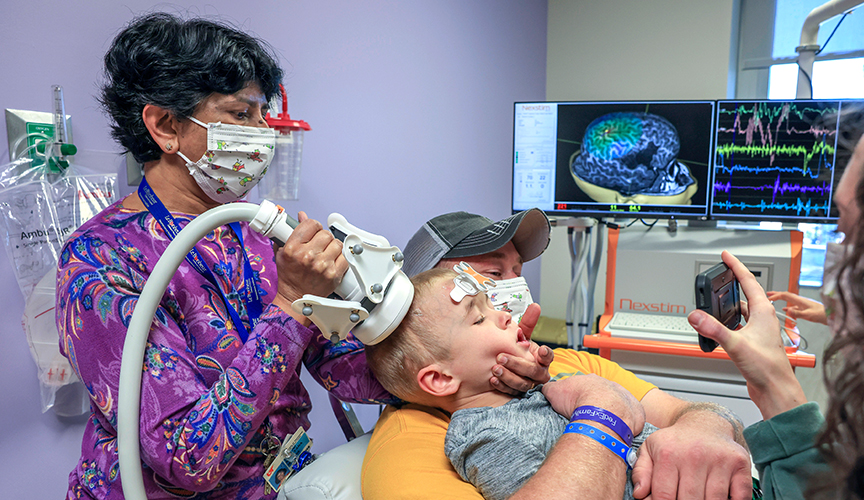
This study was a retrospective review of TMS motor and language mapping studies at Le Bonheur. Forty-seven motor mapping sessions were performed with 36 children younger than 3 years old and were successful in locating the motor cortex in 90% of children. TMS was also used to assess the risks and benefits of surgery in 11 children with lesions near the motor cortex. TMS results were used in the surgical navigation system, and motor function was preserved or improved in nine of the 11 children who underwent surgery. Two children had mild, predicted weakness after surgery.
A separate cohort of 13 children ages 5 and 6 underwent TMS language mapping, and language areas in the temporal lobes were localized in 92%. Seven of these children underwent surgery, and the TMS results provided a presurgical baseline and were used on the surgical navigation system. Post-operatively, none of the children were found to have speech or language deficits.
Overall, TMS was well-tolerated by most children and described as painless. About 20% of the children undergoing motor mapping experienced seizures during or immediately after TMS. All of the children who experienced seizures had a history of refractory epilepsy with frequent seizures, and seizures during or after TMS were consistent with their typical seizure pattern and deemed not to be directly caused by TMS.
“In our study, TMS was safely applied in young children with serious epilepsy syndromes,” said Narayana. “All our data so far indicate that the use of TMS in children is safe and effective.”
Help us provide the best care for kids.
Le Bonheur Children's Hospital depends on the generosity of friends like you to help us serve 250,000 children each year, regardless of their family’s ability to pay. Every gift helps us improve the lives of children.
Donate Now